Earlier this month, NHS England tweeted out a video to its half million followers to try to promote the Covid vaccine among children. The video cited a series of worrying, but inaccurate, statistics about the risks that Covid apparently represents to children; one in a hundred children will get sick enough with Covid to be admitted to hospital; 136 children in the UK have died of Covid-19, and 117,000 children are suffering from long covid.
The response duly ‘went viral’, attracting re-tweets from some of the biggest public health influencers online, who shared the report with their hundreds of thousands of followers, endorsing it as “an important message”, “an excellent piece”, “a great video”, and using it to lobby JCVI “when will be able to protect our children?”, and alerting people to “the misinformation out there”, no doubt with good intentions.
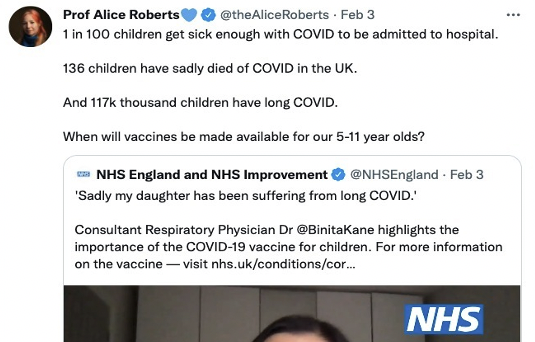
But when I watched the video I was left quite concerned and confused. As both a parent and scientist who has been involved in research on symptom duration and severity of covid in children, the cited statistics didn’t make sense to me. The idea that 1% of children with Covid are hospitalised for it didn’t pass the ‘sniff test’. I know how contentious the debates about prolonged symptoms after covid infection have been, and likewise the challenges of estimating covid mortality among children. So the idea of broadcasting confident numbers on this seemed odd, especially from NHS England.
What’s more, the powerful — and important — sharing of a story about “long covid” in a 11-year-old seemed at odds with current UK vaccination guidance, which does not currently advise vaccination of this age group. As a parent of an 8- and 6-year-old, I didn’t know what I was supposed to do with this ‘information’. Even more so when I was aware that there is not currently evidence to show that vaccination prevents “long Covid” in children.
What was even more surprising to me was the reaction from both NHS England and many commentators when I raised these points on Twitter and with NHS England directly. I previously worked in government, where every statistic that made it into official comms or a Ministerial speech came with a ‘method note’ to explain it if asked. Yet there was a deafening silence from @NHSEngland when I, and others, asked.
Several people agreed with me, sharing their working for why these numbers are at best long outdated, may be orders of magnitude out, and risk undermining confidence in vaccine communications and uptake.
But others seemed to dig in, praising both the content and tone of the messaging when challenged, and directing the discussion into an important, but different, one about the merits of extending Covid vaccination to children rather than the need for accurate and honest communication about vaccination.
My impression was that some, including influential ‘experts’, felt that the accuracy of the numbers used was secondary to advocacy objectives, i.e. the ends (promoting vaccine uptake) justified the means (using inaccurate, and emotive, statistics and powerful stories). This feels like extremely dangerous ground to me, especially given what we know about the importance of trust in vaccine confidence and uptake, and the recent worrying falls in childhood vaccination.
Having raised this with the Statistics Regulator, I was relieved to have today received the following message:
It took four days, 150,000+ views, and many hundreds of thousands of shares and impressions before NHS England finally deleted the tweet. I hope in due course these investigations will lead to improvements in the process through which statistics, especially on such an important issue as childhood vaccination, are vetted, ideally before, rather than after, publication/broadcast.










Join the discussion
Join like minded readers that support our journalism by becoming a paid subscriber
To join the discussion in the comments, become a paid subscriber.
Join like minded readers that support our journalism, read unlimited articles and enjoy other subscriber-only benefits.
Subscribe