Nature readers last summer (Photo by Michael B. Thomas/Getty Images)

In Joe Biden’s first speech following his election victory, the future President assumed the role of the nation’s doctor. Pledging to “heal America”, he promised to “marshal the forces of science and the forces of hope” to combat two viruses. The first, of course, was Covid, which has killed more than 560,000 Americans and left many more unemployed and impoverished. The second, which arose almost in tandem, is equally pernicious, if not quite so deadly: the “racism virus”.
The outbreak of this second virus was confirmed earlier this month by the Center for Disease Control (CDC) and Prevention, which issued a statement declaring racism an “epidemic” that posed a “serious public health threat”. Citing a “growing body of research”, the CDC director called on her agency — and America at large — to “confront the impact of racism”.
This is, on the face of it, a peculiar focus for America’s leading public health agency; one might think it would be preoccupied with the other pandemic ravaging the country. And yet the CDC’s statement was all too typical of today’s medical establishment. The American Psychological Association recently announced that America was “living in a racism pandemic”; the American Medical Association has called racism an “urgent public health threat”; and The Lancet has declared it a “public health crisis we can no longer ignore”.
It is easy to dismiss such rhetoric as “woke” nonsense, typical of “progressive” America’s obsession with race. But there is something striking — and troubling — about the way in which racism has evolved from a social problem into a medical one. For it is not simply a case of well-meaning medical practitioners parroting the language of social justice to “assuage their liberal guilt”, as a former member of President Biden’s Covid-19 advisory board put it. From a public health perspective, it has potentially fatal ramifications.
Take, for example, the “anti-racist agenda for medicine” recently published in The Boston Review by two Harvard doctors. In it, the pair argue that, because colour-blind solutions have failed to achieve racial equity in health care, they have had to introduce “race-explicit interventions” in their Boston hospital. These have culminated in a pilot programme of preferential care for black and “Latinx” heart failure patients, due to launch this spring; instead of triaging their patients according to the seriousness of their condition, race has become a mitigating — and deciding — factor.
In effect, it will mean that a black person with a less serious condition could be prioritised over a white patient on account of their skin colour. “Building on calls for reparations,” the two doctors explain, “we call this a vision for medical restitution.” Here, writ large at the heart of the medical establishment, was Critical Race Theory — the idea that the US is a fundamentally racist country and that race is a social construction designed to oppress and exploit people of colour.
In many ways, it was only a matter of time. As far back as 2010, the American Journal of Public Health published an article titled “Critical Race Theory, Race Equity, and Public Health: Toward Antiracism Praxis”, in which two Professors of Public Health argued that only a “race-conscious” approach to healthcare would be able to combat racial inequities. Based on “race equity and social justice principles”, they encouraged the development of solutions that “bridged gaps” in health, housing and employment.
In the years since, this medicalisation of Critical Race Theory remained purely academic, largely confined to Professors looking to rack up a few journal citations and bask in the warm glow of approval from fellow Left-wing academics. But after the death of George Floyd, that changed overnight.
As Black Lives Matter protests erupted across the country, politicians began likening the scourge of racism to a health emergency, calling it a “pandemic on a pandemic”. The mood was captured by Austin’s mayor, who cried out: “Racism is literally killing black and brown people. It’s a public health crisis, and it’s beyond time to treat it as such”.
Public health officials agreed. “While everyone is concerned about the risk of Covid,” said one infectious disease expert, “there are risks with just being black in this country that almost outweigh that sometimes”. Meanwhile Anthony Fauci, the chief medical advisor to the President who had previously denounced anti-lockdown protests, was decidedly more equivocal about BLM: “It’s a delicate balance because the reasons for demonstrating are valid, but the demonstration puts one at additional risk.”
Soon after, America’s public health bodies began discussing racism in terms formerly only used to describe Covid-19. The American Medical Association, for example, recently announced that it wanted to increase funding into the “epidemiology of risks and damages related to racism”, while the CDC’s new Racism and Health Program seeks to “build a healthier America for all” by confronting racial and health disparities.
Yet the most striking feature of these statements is their similarity. Each one promises to “acknowledge” the damaging effects of structural and systemic racism and supports the “development” of policy to combat racism.
But what does this mean in practice? In New York, for instance, the City Department of Health, in an attempt to address low testing and high positivity rates among minority communities, launched a hyper-local testing programme. It proved a success and resulted in 8,730 tests across the two postcodes. So far, so sensible.
However, compare that to the approach of the Milwaukee Health Department, which, in order to “own the work of racism being a public health issue”, devised its own “health equity initiative”. Contained within a “three-step process”, it proposed the introduction of racial equity training, the development of “a racial equity framework” and the creation of safe spaces and a “welcoming, inclusive” organisation.
This latter approach is characteristic of Critical Race Theory, which disregards evidence-led specifics in favour of ideology-based generalities. But in the field of medicine, this is particularly dangerous. American medical insurance companies, for example, now attribute lower levels of depression among black people and Latinos to under-diagnosis, even though suicide rates among white people are three times higher. Yes, depression doesn’t always manifest itself through suicide, but it is strange, as Wesley Yang notes, that Blue Cross, which provides insurance to a third of Americans, “sees ‘not enough depressed black people’ as a problem that has to be fixed”.
Elsewhere, certain states are adopting race-prioritised vaccine rollouts — a move first mooted by the CDC last year. These states, including Vermont and Montana, claim that, even after controlling for income, underlying health conditions and other variables that potentially affect the disease, there is still a racial disparity.
Put to one side the disturbing historical parallels of dividing Americans by their skin colour — it is not even clear that this racialised approach to vaccines makes sense from a public health perspective. After all, there are a number of other issues — such as education, access and outreach — that are also hindering the vaccine rollout to non-white communities. Moreover, as one former Biden official warned, it could even have the opposite effect and deter uptake if minorities fear that they are being treated like “guinea pigs”.
In reality, all that has resulted from this policy is a racially distorted vaccine rollout that is likely to fuel resentment in an already divided country. Today’s doctors are, of course, doubtlessly well-intentioned in their attempts to cure America’s societal ills. But shifting attitudes on race is a long and difficult process — and not something that can be remedied with a three-step public health initiative.





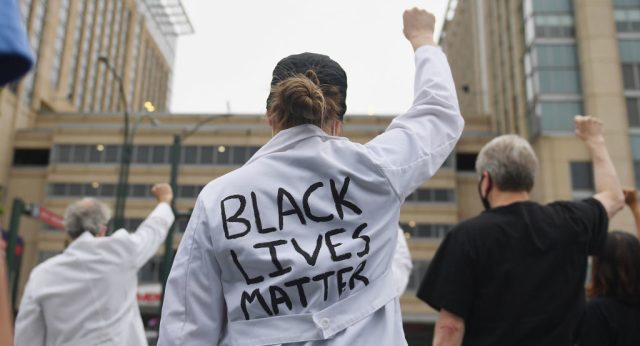




Join the discussion
Join like minded readers that support our journalism by becoming a paid subscriber
To join the discussion in the comments, become a paid subscriber.
Join like minded readers that support our journalism, read unlimited articles and enjoy other subscriber-only benefits.
Subscribe