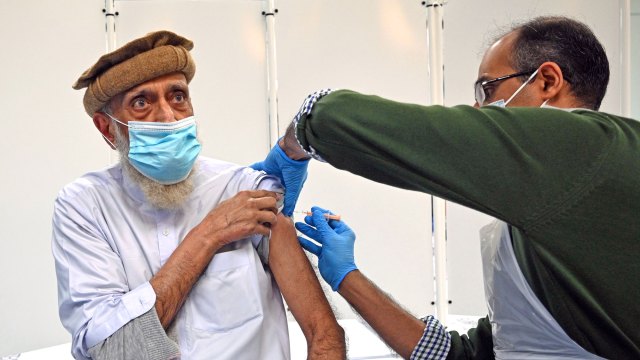
More vaccine uptake is needed Oli Scarff/AFP via Getty

Matt Hancock stood up in the Commons yesterday to congratulate himself and the Government on how well it had done recently. More than 2,000 cases of the new “Indian” variant have been detected, nearly 500 of them in Bolton and Blackburn, but Hancock was pleased to tell everyone that he has sent thousands of vaccination and testing staff to the areas, and to Bedford, where there’s another outbreak.
It’s inconvenient timing, given that England has just relaxed restrictions, and the Health Secretary didn’t seem overly keen to talk about the Government’s failure to impose restrictions on travel from India for several weeks after the new variant was known to be causing havoc in south Asia. But he made one interesting point: the majority of people in Bolton and Blackburn who are in hospital with the new variant are of an age who are eligible to have the vaccine, but who have chosen not to.
That is true. And apparently there are “growing concerns” in Downing Street that even a small number of people refusing Covid vaccines could delay the final restrictions in June. Hancock didn’t say it, but there does seem to be an attitude among some people, not just in Government, that vaccine-hesitant people have made their bed and now they need to lie in it. They’ve been offered the jab, they’ve turned it down, and it’s now their own problem.
That’s understandable. After all, the most prominent vaccine sceptics are crankish academics and Jeremy Corbyn’s brother, Piers — although Jeremy himself doesn’t seem completely on board the vaccine train either.
But while the middle-class dinner-party sceptics get the most attention, vaccine hesitancy is actually highest in other demographic groups — notably, ethnic minorities and the most deprived. While more than 90% of Britons over 50 have had at least one jab — and the British are the least vaccine-sceptical nation in the world — coverage varies widely by ethnicity. By April, people of white British or Indian heritage had over 90% take up; but people of Pakistani origin had just 78%, and black African and black Caribbean groups were down at 71% and 67% respectively.
There’s a socioeconomic difference, as well, although it’s not so pronounced. Only 87% of people in the most deprived 20% of the population were vaccinated, compared to 95% of the richest 20%.
And while it’s tempting to say that if people aren’t getting vaccinated, it’s their own fault and their own problem, it’s not entirely true. People don’t usually choose the communities they grow up in, and if you live in one where lots of people don’t trust the British establishment for whatever reason, I don’t think it’s fair to say that it’s your own fault.
And it’s certainly not just their problem, either. Most of the population has been vaccinated, meaning that it will be increasingly hard for the virus to spread and even harder for it to kill people. But the coverage is highly uneven. People tend to live in communities full of people roughly like themselves — with similar socioeconomic and ethnic status. That means there will be lots of places in the UK with large numbers of unvaccinated people of vulnerable age.
According to Dr Adam Kucharski, a mathematical epidemiologist at the London School of Hygiene and Tropical Medicine, the future of the pandemic in the UK is likely not to be huge national outbreaks, but more localised. “It’s worth getting away from the average national coverage,” he says. “It won’t come averaged across the whole UK; it’ll be clusters.”
And if there’s a cluster, local healthcare systems can be overwhelmed, even if the UK system as a whole has plenty of spare capacity. As we know, when Covid overwhelms healthcare systems, people die who wouldn’t otherwise have had to, and it’s not jot just Covid patients: “People who are in car accidents can’t get the care they would otherwise have had,” says Dr Duncan Robertson, a policy researcher focusing on Covid modelling at Loughborough University. Or cancer patients, or people having heart attacks, or whatever. Plus, while the vaccines are very good, they’re not perfect: some vaccinated people will still die as a result of other people’s refusal to take the vaccine. If a very large number of people get the vaccine, a small percentage of them will die, and a small percentage of a very large number is still a large number.
The new variant seems to be about 50% more transmissible even than the Kent variant, which means that we need to vaccinate many more people than we would have done to achieve herd immunity, and that it will spread much more quickly around susceptible people than earlier variants did.
It’s worth remembering that, on one level, this is a good problem to have, and the UK is still in an amazingly strong situation. And although the Indian variant has thrown a bit of a spanner in the works, it’s still time to start thinking seriously about when we start donating vaccines in large numbers to the rest of the world — not just pledging them but actually giving them. The Novavax factory in Middlesbrough should come online soon and that might be a good time to start offering them around.
Obviously the British Government has a responsibility to UK citizens, but even from a purely self-interested point of view, quite soon there will come a point at which a vaccine dose will do more good for the UK if it’s in the arm of an Indian citizen than a British one. We live in an interconnected world: variants can get here easily from anywhere, and a crippled world economy is bad for us, too. We are still doing amazingly well with our vaccination programme, and it may be that we can soon start to afford to be generous.
But also, this is a huge reason to really push on with the vaccination campaign, and to especially focus on ethnic-minority groups. One senior scientist I spoke to said that some of the things we can do are pretty obvious, like finding healthcare providers who can speak the predominant minority language in affected areas. They’re not necessarily easy — Urdu-speaking health professionals don’t grow on trees — but we ought to try.
Most importantly: while I understand Hancock’s eagerness to say that most of the people who are in hospital have chosen not to get the vaccine in the end, vaccine scepticism is everyone’s problem, not just the sceptics themselves. Britain is ending lockdown — that’s great — but even a relatively small number of vaccine sceptics, if they’re clustered enough, could make the opening-up go very badly wrong.









Join the discussion
Join like minded readers that support our journalism by becoming a paid subscriber
To join the discussion in the comments, become a paid subscriber.
Join like minded readers that support our journalism, read unlimited articles and enjoy other subscriber-only benefits.
Subscribe