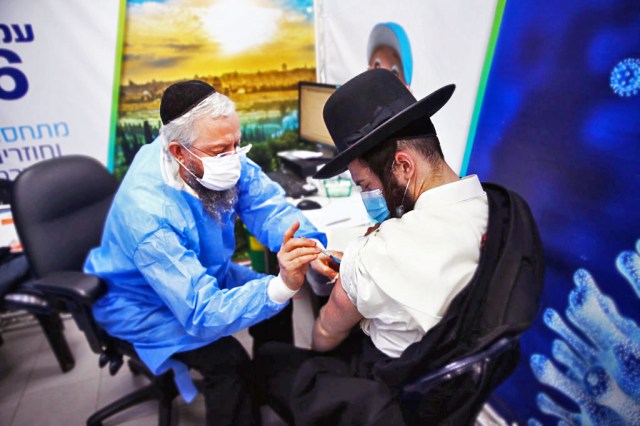
Did Israel get lucky? (Photo by Mostafa Alkharouf/Anadolu Agency via Getty Images)

Israel’s remarkable vaccination success story might be less interesting if it were only pulling slightly ahead of comparable countries. But the difference is not one of degree. With more than 82 doses delivered per 100 citizens by the end of last week — compared with 26 for the UK, 17 for the US, and a scandalous 5.9 for the EU — Israel is significantly ahead of the pack.
But why is that? No doubt that’s the question governments across the world are currently attempting to answer, in the hope of replicating some of Israel’s success. But the truth is that the country’s vaccination rollout has been a unique victory — one that has emerged from a confluence of factors which, while individually common in other countries, Israel is alone in having.
Some of those factors are structural. Israel’s universal health system, for example, is built on a regulated service provided by four competing non-profit health service organisations, called “sick funds” — a bit like having four versions of the NHS. Every resident must be a member of a fund, which are financed by a small progressive health tax that ranges from 3-5% of a person’s income. In effect, the system combines the benefits of universal coverage with competition, though it is hardly alone in the world in doing so.
Far less common, though, is the extent of digitisation in the Israeli health system. Each fund maintains a fully digitised records and appointments system, integrated with smartphone apps, websites, and automated phone systems. Crucially, these records are directly connected to the Ministry of Health’s universal vaccination database. This meant that when the time came for organising Covid vaccination appointments, there was no new infrastructure to set up. Appointments were organised automatically for the people who most urgently needed them on platforms that were already familiar.
But none of that would have mattered without an adequate vaccine supply. And this is where the Israeli government stepped in. Well before any vaccines were approved, senior officials were already signing deals with Moderna, Pfizer, AstraZeneca and others — as well as funding a domestically produced vaccine, which is still in clinical trials. They also began securing a large supply of syringes and needles, an element of the vaccine strategy which was surprisingly overlooked by other countries, most notably Japan.
Of course, many countries put in early bids for vaccines before they were tested or approved. But while EU procurement was focused on leveraging the bloc’s enormous purchasing power to lower the price of vaccines, the Israelis knew there was little hope that a small peripheral country could drive a hard bargain. Working on the assumption that the costs of further lockdowns and hospitalisations would dwarf an inflated vaccine price, Israel prioritised buying as much of it as possible in the swiftest period of time. Exact figures are yet to be made public, but reports in the Israeli press suggests the government paid between double and triple the going rate.
Yet Israel did not just offer more money to get to the front of the queue. It also offered pharmaceutical companies anonymised real-time data on vaccine distribution, side effects, and efficacy — in effect turning its population into Phase IV trial. Data on this scale goes far beyond anything drug companies could obtain in even the largest clinical trials.
Still, while an adequate supply is crucial for a successful vaccination program, it hardly guarantees one. Indeed, it is Israel’s logistical operation, rather than its digitised record system and political decision-making, that ultimately ensured the country’s vaccination program was a success.
As soon as the vaccines arrive at Israel’s Ben Gurion Airport, they are taken straight to a centralised ultra-freeze facility just outside the airport. From there, three times a week, coordinated shipments of vaccine pallets are sent out to the four Israeli health organisations, as well as hospitals, prisons, army bases, purpose-built centres, drive-through facilities, and even mobile units stationed on weekend hiking trails. All are staffed by nurses from local hospitals and clinics which have seen reduced demand during the pandemic, as well as by paramedics and those specially trained to provide extra capacity in the months before the first vaccines arrived.
These centres process, on average, at least eight patients per hour per nurse. Last week, that meant that more than half of Israelis have received their first dose and more than a third have already received both — a figure made even more impressive when you consider that 30% of the population are under 16 and therefore ineligible for any vaccine (pending clinical trials on younger subjects).
Israel’s approach has also adapted when necessary. Early on, a call centre to report possible side effects was established to prevent the telephone appointment system being clogged up and, even more important, to reduce A&E visits to a bare minimum. Meanwhile, messaging for Israel’s diverse population has become more targeted: faced with low turnout in the first weeks in the Arab and ultra-Orthodox communities, authorities turned to social media and other outlets with tailored messages.
But, given that much of Israel’s vaccine roll-out benefitted from pre-existing infrastructure and policy decisions that are now too late to copy, is there anything that other countries can still do to try and replicate some of its success? The simple answer is: nobody knows for certain. But regardless of how easy they are to copy, there are two aspects of Israel’s vaccine operation that bear noting.
First, the criteria for the initial rollout were very broad and very simple. There was no list of at-risk professions and no list of pre-existing medical conditions that meant certain people were prioritised. Had there been, it’s safe to assume that call centres would have been deluged by those seeking exceptions, exemptions or early appointments. Instead, anyone over the age of 60 — a much lower cut-off than any other country — was invited to get vaccinated in the first three weeks, together with medical staff and anyone in “institutionalised” living (mostly care homes).
Though people in their 60s are not at a significantly high risk of dying from Covid, by vaccinating them early, the Israeli health organisations attended to most of the relevant pre-existing conditions, particularly diabetes and obesity. “The low initial age minimum covered nearly all of the co-morbidities anyway,” Dr Boaz Lev, who heads the Ministry of Health’s Advisory Committee on Pandemics and Vaccines, told me. “And it generated early momentum in a way that stricter criteria could not have.”
Such simple criteria were easy to understand and hard to resent. And the result was that, in the first month that vaccines were available, Israel and Denmark were the only countries where supply actually became an issue. In the rest of Europe and North America, unused vaccines sat in freezers or, worse still, thrown away.
Which brings us to the second crucial aspect of the Israeli operation that observing governments should take to heart: from the very beginning, there was a strict policy of no wastage. Indeed, if there’s one motif to the entire Israeli effort, it’s the idea that one discarded vaccine constitutes a systemic failure. This meant that in small towns where there were leftover vials at the end of the day, residents received text messages inviting them to be vaccinated. Anyone near a vaccination centre where too many vials had been defrosted was also encouraged to get a jab. Even people under 60 could show up at the end of the day and, in the event that there were extra doses, could get vaccinated.
The no wastage policy has had three benefits. It will save money in the long term, as fewer vaccines will need to be purchased than would have been the case if many had been spoiled and discarded. It relieved pressure on the appointments system by discreetly giving vaccines to those people who, for whatever reasons, wanted them earlier than the criteria would allow and who would otherwise have burdened the system with phone calls. And, perhaps most importantly, it quickly introduced more of the vaccine into the community much earlier than would otherwise have been the case — thereby reducing the virus’s transmissibility.
What’s remarkable about this most Israeli aspect of the whole Israeli operation is how little consideration was given to it. When I approached officials from the sick funds, the Ministry of Health, and nurses on site with questions about the no wastage policy, they all spoke of it as being common sense; something almost automatic. Israelis who hear the story of Hassan Gokal, the Texas doctor fired for ensuring ten thawed doses would be injected rather than discarded, assume that they have stepped through the looking glass.
These aren’t, of course, logistical innovations that stand alone. A low minimum age at rollout can only really work where the initial supply is suitably large, and a policy of no wastage is only conceivable in a system of fully integrated and readily accessible digital records. In Israel, a leftover dose could be given to someone who happened by a vaccination facility because the nurse was able to swipe that person’s magnetic medical card and see that they have no allergies, no contraindications for the vaccine, no positive tests for the virus — and the person would leave with the appointment for the second dose already booked in the system.
It’s also worth noting that, in retrospect, Israel’s decision to push hard in the first three weeks was also a huge gamble. Indeed, it might have been more prudent in the first weeks of the vaccine rollout to ensure that they went only to those most acutely in need — those over 80, overweight, and over in assisted living facilities. No one knew for sure there would be a steady supply after the first batch.
But, as it turned out, it was the momentum of those initial three weeks and the reliable data it provided that convinced Pfizer and others that a steady airlift to Israel was worth their while. Before this was settled, it seemed that Israel might even have to pause first doses after the third week doses until further shipments could be secured.
As it turned out, talk of a vaccine shortage spurred even more people to show up, as citizens began to worry that they might end up waiting until late February or March to be eligible again. “I swear we didn’t plan it that way,” an official from the Ministry of Health who worked on a number of the vaccination PR campaigns told me. “But the truth is, it did more to sustain momentum and interest than any of the influencers we contracted.”
The question for Israel now is whether it can complete the task. Pandemic fatigue has set in, and the most recent lockdown has already been lifted despite the infection rate remaining far higher than it was when either of the previous two lockdowns were ended. And while Israel’s dense population and efficient public health system have proved invaluable, some of its demographic problems will be challenging to surmount. Vaccination rates are still lower in the Arab and ultra-Orthodox communities, precisely the places where infection rates are higher.
An even bigger challenge is Israel’s young population. Even if all Israeli adults were vaccinated, that would only amount to about 70% of the population, far below what experts estimate is necessary for herd immunity. By summer it is believed that a vaccine will be approved for those aged 12 and up, but the incentive structure for vaccinations will be flipped.
It is easy to persuade vulnerable 80-year-olds to sign up for a vaccine for a disease that might kill them. Whether parents of teenagers will be similarly inclined for an injection that, while absolutely necessary for society at large, only protects their child from what is likely a minor illness, remains to be seen. Meanwhile, for the rest of the world, such a dilemma is yet another cause for envy.









Join the discussion
Join like minded readers that support our journalism by becoming a paid subscriber
To join the discussion in the comments, become a paid subscriber.
Join like minded readers that support our journalism, read unlimited articles and enjoy other subscriber-only benefits.
Subscribe