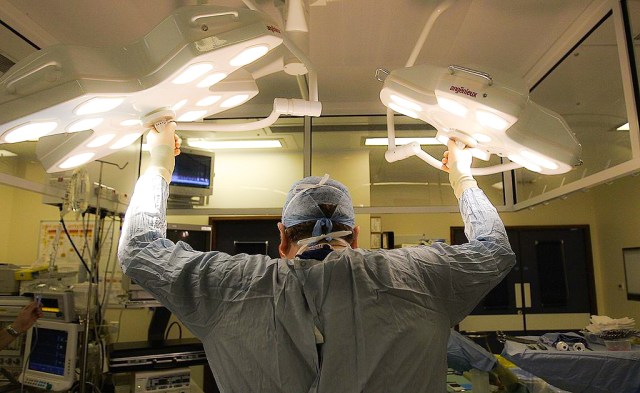
“You have to shake the system by challenging it.” Credit: Christopher Furlong/Getty

They say the first step in fixing a crisis is to recognise there is a problem. So let us give thanks for a Labour leader’s dismissal of the belief that Britain’s health service is the envy of the world — a deluded concept that, in the words of Sir Keir Starmer, is “plainly wrong”. Yes, he was adopting Blairite tactics to confound expectations with a bit of political cross-dressing, while also obviously aware of polls showing the drastic collapse of faith among voters in their once-worshiped NHS. His reform plans are rudimentary, his funding suggestions sketchy and his proposal to nationalise general practitioners seems ill-conceived. Yet this is still an important moment.
Britain has clung for so long to this weird comfort blanket, the risible idea that the rest of the world was looking with longing at a health system that has been in crisis for much of its 75-year history. For more than two decades I have argued that such blinkered worship of the NHS and deification of its staff was highly corrosive, since it frustrated reform, intimidated politicians and silenced criticism. The result has been a series of grotesque patient safety scandals — usually with agonising or fatal consequences affecting the most marginalised groups in society — and dire outcomes in many key areas, from cancer to infant mortality, compared with other rich nations.
Now the crisis has exploded, costing thousands more lives amid delays, strikes and staff shortages. Yet why is anyone surprised given the grim lack of reality that has swirled around the NHS for so long? I was a lonely voice pointing out the absurdity of Danny Boyle’s 20-minute homage to a flawed public service in the 2012 London Olympics opening ceremony with its dancing doctors and bouncing babies. Such misty-eyed myopia, especially prevalent on the Left, led to great excitement among devotees two years later when a US body ranked the NHS first among 11 health systems largely on grounds of access and efficiency. Yet even The Guardian report — headlined NHS comes top in healthcare survey — admitted that “the only serious black mark against the NHS was its poor record on keeping people alive”.
This failure to prevent needless deaths felt to me like a rather fundamental failing for a health service. It was confirmed by a damning inquiry by four respected think tanks to mark the NHS’s 70th birthday which found Britain had among the worst “amenable mortality” levels — when people die from potentially preventable conditions — among 18 similar nations. They pointed out how 117 out of every 100,000 Britons died avoidably in one year under study, compared with just 78 in best-performing France. This pivotal report also found Britain spending almost the average on health for rich nations. Since then, NHS England alone has seen its funding rise another £38bn.
My personal puncturing of the NHS mythology came with the birth of a daughter discovered to have profound disabilities and health concerns. This sent my family hurtling into the hell of its underbelly, glimpsing the arrogance, inertia, insensitivity and waste lurking beneath the sanctified image. I have never forgotten our first visit to Great Ormond Street and hearing a receptionist cheerily say “Didn’t anyone tell you — your appointment’s been cancelled?” to a desperately-worried young couple who had travelled down from the north-east with their tiny sick baby. Then came years of battling bureaucracy — answering the same questions over and over again — while witnessing blunders, fighting lethargy and dealing with medical egos.
As the parent of another disabled child told me after watching that risible Olympic spectacle, how sickening to endlessly hear mantras of praise for the NHS from people whose lives were not engulfed in a daily struggle against its inertia and ineptitude to protect the life of someone precious. Today, we do everything possible to keep my daughter out of hospital. Yet she has survived almost into her thirties despite a life-threatening condition thanks to my wife’s strength, the wonders of medicine and the support of many superb carers, doctors, nurses and therapists. We have seen both the best and the worst of our system over the years.
The NHS problems have been glaringly obvious for years. It is an institution created after the Second World War and designed for a different era, focused on the fight against infant mortality, infectious disease and industrial injuries. It was built around big hospitals, dominant male consultants and demands of doctors; remember Nye Bevan’s infamous pledge to “stuff their mouths with gold” to overcome opposition to his socialised system. But many of the original battles are won, our population has aged, medicine advanced and society changed. The core concerns now are those linked to ageing or disability, often involving chronic conditions with co-morbidities, alongside an explosion of obesity and mental health problems being seen from an alarmingly early age.
These are the old, complex and chronically-sick patients soaking up more than two-thirds of health spending, not the higher-profile emergencies that the NHS usually handles so adroitly if people can find an ambulance. People such as my daughter — or my father, who died, aged 97, after his long decline with dementia. This has been recognised for years. There have been repeated demands for a shift from hospitals towards expanded community services that combine primary and secondary care services. Now Labour is reheating Lord Darzi’s proposal for London polyclinics and applying a version of it nationwide to unite GPs, diagnostics, therapists, community nursing and mental health teams under one roof — but he first raised this idea 15 years ago.
The harsh truth is that far from being the envy of the world, no one setting up a health system would adopt our current system. I know eastern European carers so horrified by the NHS that they fly home if needing to see a doctor or dentist. As a journalist investigating care, patient safety and mental health provision, I have written about too many disturbing, routine and fatal failings in the NHS heart. One government study sparked by Sara Ryan, a mother who became a campaigner after her teenage son died in terrible circumstances, found citizens with learning disabilities likely to die 26 years earlier than their peers — with medical errors involved in one in eight of the fatalities examined.
My exposés of the barbaric treatment of autistic people and citizens with learning disabilities, let down by a dysfunctional care system and stuffed into abusive detention in hideous psychiatric units for many years, led to five inquiries, endless promises of action, personal awards — but nothing changed. Other victims of NHS failures tend to be elderly people, as revealed most notoriously with the inquiry into hundreds of deaths in disgraceful conditions in two mid-Staffordshire hospitals, and female patients. “Our healthcare system disproportionately fails to listen to women and keep them safe”, admitted the Government last two years ago in response to three more horrific treatment scandals.
Now we face the question of how to salvage a health service that seems to have reached breaking point on so many fronts. Sadly, much of this debate remains glib, self-serving or stuck in the past. It is dominated by doctors, with constant calls for more cash and complaints about their pressures while they pose as protectors of the NHS. Yet we should not forget that when Tony Blair drove up health spending, much of the money was grabbed by GPs. A British Medical Association negotiator later said their salaries soared 60% in three years as he boasted how the Government let them drop out-of-hours cover in return for a small pay cut they considered “a bit of a laugh”. Few patients laugh today when struggling to access local practices. NHS data, however, shows the number of doctors has risen almost one-third over the past 12 years of supposed Tory “austerity”.
Cash is, of course, a significant factor in health care. Yet when I first began looking into these issues at the turn of this century, I was struck to see spending levels one-fifth higher per capita in Scotland than in England and close to the European average. There were, proportionately, almost one-third more consultants, nurses, general practitioners and acute beds than south of the border. But it also had longer waiting-lists, lengthening waiting times and death rates for big killers such as heart disease, cancer and strokes among the worst in developed nations — which even a Scottish Labour minister admitted to me was not all down to drink and poor diet.
Our leaders have failed spectacularly to rise to this critical national challenge. Politicians pander to medical unions on pay, to food industry lobbyists on obesity measures, and to local voters over threatened hospital closures. They call for “reform” or “modernisation”, yet offer ideas dismally small in scale — as symbolised by Rishi Sunak’s suggestion during the Tory leadership campaign of a £10 fine for missing a GP appointment to help cure the NHS. There are broadsides against managers, who comprise an unusually small slice of a health workforce in the NHS and are essential to its smooth running; indeed, hiring a few more might relieve frontline medics of some of the bureaucracy that soaks up too much of their time, especially if they have clinical experience. Now some commentators call for a switch to a social insurance model, but inevitably fail to explain how such a huge, disruptive reform might be achieved without bureaucratic and patient chaos.
Then there is the bogeyman of “privatisation”, a thorny issue that underscores the pitiful nature of debate. Private contractors, from GPs through to caterers, cleaners and technicians, exist across the NHS. In the year before Covid, they carried out half a million elective surgeries with highest patient approval ratings. One eye surgeon told me he could perform three times more cataract operations in his private work, freed from NHS bureaucracy and the need to chat so much with patients. At the same time, some repulsive profiteers have filled the gaping holes in psychiatric services, leading to sickening abuse, needless deaths and routinely-wasted resources. They expose complacent commissioning and gross regulatory failures.
There can be good and bad in any organisation, whether public or private, and we need to harness the best of both while protecting patients far better. I was struck when visiting Hinchingbrooke Hospital in Huntingdon — briefly handed to a private firm before this unusually bold experiment was killed by political foes — to witness intriguing insights into innovation, procurement and staff empowerment. This 304-bed district hospital cut out £11m in costs over two years, which included a £3m saving by abandoning the NHS bulk purchasing system for supplies while also handing more financial responsibility to frontline staff. “You have to shake the system by challenging it,” said the doctor running the hospital, a former opponent of privatisation. “And you can only challenge it if you let fresh ideas come in.”
The painful reality is a need to build on existing foundations. Yet we cannot keep pouring in an ever-greater share of state resources to a floundering institution. The Nuffield Trust pointed out last year that the department of health and social care’s budget has doubled as a share of GDP since Margaret Thatcher took office. By the end of this parliament, it will consume four in ten pounds of the Government’s daily spending. Partly this is down to substantial population growth and amazing medical advances. But the key issue is age. The proportion of our population over 85 has doubled in three decades while the share of citizenry in their early twenties shrunk more than one fifth. These older folks use ten times more hospital resources. Now throw in all those other issues such as the post-Covid rise in long-term sick, a near-doubling in obesity over three decades and how the fastest-rising demand for social care is coming from working age adults, often with chronic and complex conditions.
Such problems, faced also by almost all other wealthy nations, are immense. But they need to be tackled since they affect the economy and millions of families. I have suggested that our new monarch has his first royal commission to grapple with the issues. But my enthusiasm waned after seeing this week’s launch of The Times health commission — an interesting and laudable idea undermined by its familiar line-up of doctors, academics, businessmen, professors and policy wonks. No patient commissioners, let alone any of the campaigners who exposed safety scandals after suffering horrors. No one from the care sector. It even includes Dame Clare Gerada, president of the Royal College of GPs, who advises a lamentable private firm behind some of those abusive detentions, regulatory failures and fatalities but refuses to discuss her role or remuneration.
There is no simple panacea. But sticking plaster politics can no longer cover the festering wounds. So I would offer three key suggestions for discussion.
First, and most important, we must stop treating social care as a second-class public service. This intensifies pressures across the NHS, yet the problems are largely ignored except through the prism of elderly bed blockers and middle-class home owners forced to sell properties to fund elderly care. When Covid struck, real-term spending on social care was £300m lower than a decade earlier despite all those billions pumped into the hallowed NHS. Local authorities were among the biggest real victims of austerity. No wonder there are catastrophic and rising staff shortages — inflamed by Brexit, as I have seen with my family — because of the appalling low pay of carers, despite their vital role in society. Yet still some fat cat firms and private equity vultures are allowed to cream off millions into tax havens.
But it is not just about pay. It is, of course, shameful that people earn more stacking shelves in a supermarket than assisting other citizens to lead their most fulfilling lives. This must be rectified. Yet I know of care jobs going unfilled for months despite paying more than twice usual rates. The pandemic exposed society’s attitudes towards elderly and disabled people when thousands of old folks were discarded from hospitals to “protect the NHS”, then blanket “Do Not Resuscitate” orders were imposed without consultation. Britain lacks compassion for its most vulnerable citizens. The Government has finally started to funnel in a bit more cash, but this societal attitude has left the care system disintegrating and hard-working staff with shockingly low status.
Corrosion of the care system not only traps elderly patients in hospital, but it leaves many desperate people with unmet needs as 14,000 requests for help are rejected daily. So conditions deteriorate, stresses shatter families and ultimately spending ends up far higher. Consider this simple equation: a teenager with undetected or unsupported autism who ends up in a secure psychiatric unit can cost the NHS £13,000 a week and the average length of incarceration is more than five years. It would be so much cheaper and more humane to fund a functioning care system.
This links to another fundamental issue. The need to build community services adopting a more holistic approach is most pressing in mental health, where state failures, short-sighted cuts and consequent shrivelling of provision mean concerns — especially at the most serious end of the spectrum — often go untreated until they explode. Even children can wait up to three years to access services, which only fuels their anxieties and can have life-long consequences. We have ended up with a hollowed-out system that starts with overloaded GPs doling out too many drugs — and can end with people needlessly locked up in those hideously-expensive secure units that are horribly over-reliant on pharmaceutical and physical restraint.
Then, thirdly, there is the delicate issue of end-of-life care. I am opposed to euthanasia, not on moral or religious grounds but — having investigated its usage in Belgium — from fears over protection of vulnerable people and the inevitability that laws gradually become more permissive. After all, if permitted for physical pain, why not for mental suffering? I would far rather see hefty investment in our fantastic palliative care and hospices. But this is a valid debate on both ethical and financial grounds. It has been suggested in the US that one-quarter of health spending goes on people in their last year of life, although others argue the figure is lower. Certainly huge sums go to sustain patients in their fading twilight for a few more months.
The US doctor Atul Gawande has written movingly about the medicalisation of mortality and lack of dignity in death. Now this issue has been stirred up by the oncologist Ezekiel Emanuel, an adviser to two presidents, disclosing that he will reject all medical treatments from the age of 75. “Death is a loss,” he wrote. “But here is a simple truth that many of us seem to resist: living too long is also a loss.” He argues that extending life through a barrage of treatments leaves many people in a deprived and often-lonely state as they decline, so his solution is to let nature take its course. This is a radical proposal. Yet some doctors privately say they would refuse many treatments they recommend for patients nearing the end of their time. Maybe we need to talk more about the best way to die as well as saving lives.
There are many other ways to improve the NHS. Technology is one obvious way to reduce the workload for medics and avoid mistakes. Although GPs have largely switched to effective digital records, many hospitals remain in the dark ages. Blair blew £12bn on a bungled attempt to integrate systems. When Jeremy Hunt became health secretary in 2012, the NHS was the world’s biggest buyer of fax machines so he pledged to make it paperless by 2018. Then his successor Matt Hancock failed in his own pledge to ban them by 2020. Some hospitals have several IT systems; such is the confusion, they rely on paper. It is claimed junior doctors can spend almost half their time on tasks that could be largely automated.
Last year, I reported on Estonia’s impressive embrace of digital government. This includes a fully-digitalised health service — ironically, based on Blair’s abandoned system. Any medic can instantly access a patient’s history anywhere, drugs get automatically cross-checked for safety — yet patients control their records. If they want to seek a second opinion, they can block a look at their initial diagnosis. And they can track treatment and spending in a system similar to the NHS, which helps reduce padding of bills and reminds them that every call, consultation or test has a cost. Peeter Ross, a radiologist and e-health expert, admitted there was resistance at first. “Doctors are trained to think they’re the experts who make decisions but this is patient data,” he said. “We must be equal partners. This works better for us all.”
This underlines the need for cultural change, increasingly recognised by many doctors, especially from younger generations — and this includes the urgent need to drive out a toxic culture of cover-up. The NHS should cherish, rather than crush, whistle-blowers raising concerns. Any system reliant on human beings will make mistakes, especially when under pressure. But it needs to learn the lessons to avoid subsequent grief and pain. This is recognised by the airline industry. But the NHS reaction is all too often to silence complainants, sweep concerns under the carpet and summon lawyers from fear of litigation. This can result in long, drawn out and distressing legal battles. The only beneficiaries are lawyers, who pocketed about one quarter of the £2.5bn spent by the NHS last year settling claims.
There are many other incremental ideas to help revive the NHS. But let us celebrate this moment as Labour finally accepts that the NHS is a flawed institution rather than a shining light of British exceptionalism. Reality is dawning in Westminster in response to the growing public and professional anxiety. We need to have honest discussions about how our country funds and runs our health and care systems — and who it serves. Some solutions are obvious, such as more effective use of technology and transparency. Others stray into the difficult terrain of payments, profits and even the meaning of life and death. One thing is clear, though: salvation for the NHS must revolve around patients, not just professionals.









Join the discussion
Join like minded readers that support our journalism by becoming a paid subscriber
To join the discussion in the comments, become a paid subscriber.
Join like minded readers that support our journalism, read unlimited articles and enjoy other subscriber-only benefits.
Subscribe